Picture your most seasoned claims adjuster. Now, imagine they could read, sort, and make sense of thousands of pages in just a few minutes. That’s not science fiction anymore—it's the reality of AI insurance claims processing. This technology uses intelligent systems to automate and speed up the entire claims journey, from the first call to the final check.
The New Reality of Insurance Claims
For decades, the claims process has been a notorious bottleneck—slow, manual, and drowning in paper. Adjusters, third-party administrators (TPAs), and legal teams have burned countless hours on low-value work like sifting through documents, keying in data by hand, and flagging potential issues. It's an approach that’s not just inefficient but also ripe for human error, creating delays that frustrate customers and bloat operational costs.
Think of the old way as a library where a single librarian has to find, read, and cross-reference every book manually. It’s a painstaking process that always leads to backlogs and missed details. AI insurance claims processing completely flips that script.
From Manual Labor to Intelligent Automation
AI acts like a team of digital expert assistants, working around the clock. It takes in a flood of unstructured data—photos, police reports, medical records, policy documents—and instantly gets it organized. This isn't just a minor tweak; it’s a fundamental operational overhaul. Instead of spending 80% of their time on administrative tasks, adjusters can now focus on what truly matters: complex decision-making, negotiation, and talking to customers.
This shift is driven by a few massive improvements:
Speed: AI slashes the time it takes to review and process documents, dramatically cutting down claim cycle times.
Accuracy: By automating the process, you minimize the risk of human error in data entry and analysis, leading to far more consistent and reliable outcomes.
Insight: AI spots patterns, red flags, and missing information that a human reviewer, buried in a mountain of paperwork, could easily miss.
For P&C carriers, TPAs, and legal firms, this moves claims management from being a reactive, labor-intensive cost center to a proactive, data-driven strategic function. The goal shifts from just processing claims to resolving them with maximum efficiency and precision.
Traditional vs AI-Powered Claims Processing at a Glance
To really see the difference, it helps to put the old and new methods side-by-side. The traditional approach is linear and plagued by manual handoffs, while the AI-powered model is fast, integrated, and intelligent. For a deeper dive into these modern approaches, check out our guide on 2025 trends in claims management and automation.
The table below gives you a clear snapshot of how much has changed.
Claim Stage | Traditional Manual Process | AI-Powered Process |
|---|---|---|
Intake | Manual data entry from emails, faxes, and portals. High potential for errors and delays. | Automated ingestion and data extraction from all sources into a single, unified system. |
Review | Adjusters manually read through hundreds of pages to identify relevant information. | AI tags key evidence, identifies risk factors, and flags missing documents in minutes. |
Settlement | A lengthy process involving multiple handoffs, potential rework, and slow communication cycles. | AI-driven insights and drafting tools accelerate decisions, enabling resolutions up to 4x faster. |
The contrast is stark. One path is defined by friction and manual effort; the other by speed and intelligent automation. This isn't just about doing the same things faster—it's about fundamentally changing how claims are handled from day one.
How AI Actually Transforms the Claims Workflow
To really get what AI does for claims, you need to stop thinking of it as one magic button. It's more like a series of smart, connected steps that create a completely new workflow, right from the moment a claim is filed. The system acts like a seasoned paralegal—one that can ingest thousands of documents and instantly organize them into a clean, audit-ready file.
This isn't just theory; it’s driving massive operational shifts. The global AI insurance market is expected to rocket from $8.6 billion in 2025 to nearly $59.5 billion by 2033. That growth is fueled by AI's power to untangle claims, with real-world results like slashing document collection time by 77% and closing cases up to 4x faster.
Step 1: Intelligent Document Intake and Centralization
The first stage of any claim is pure chaos. Documents flood in from everywhere—emails, client portals, direct uploads—and in every format imaginable, from PDFs and photos to messy scanned forms. In the old days, an adjuster or an assistant would have to manually download, rename, and file every single piece of paper.
AI-powered intake completely automates this mess. The system becomes a central hub, grabbing every document and pulling it into a single, unified workspace. More importantly, it starts keeping tabs on what's there—and what's not—right from the get-go, creating an instant inventory.
The diagram below shows the stark difference between the old, slow manual workflow and the fast, parallel processing that AI makes possible.
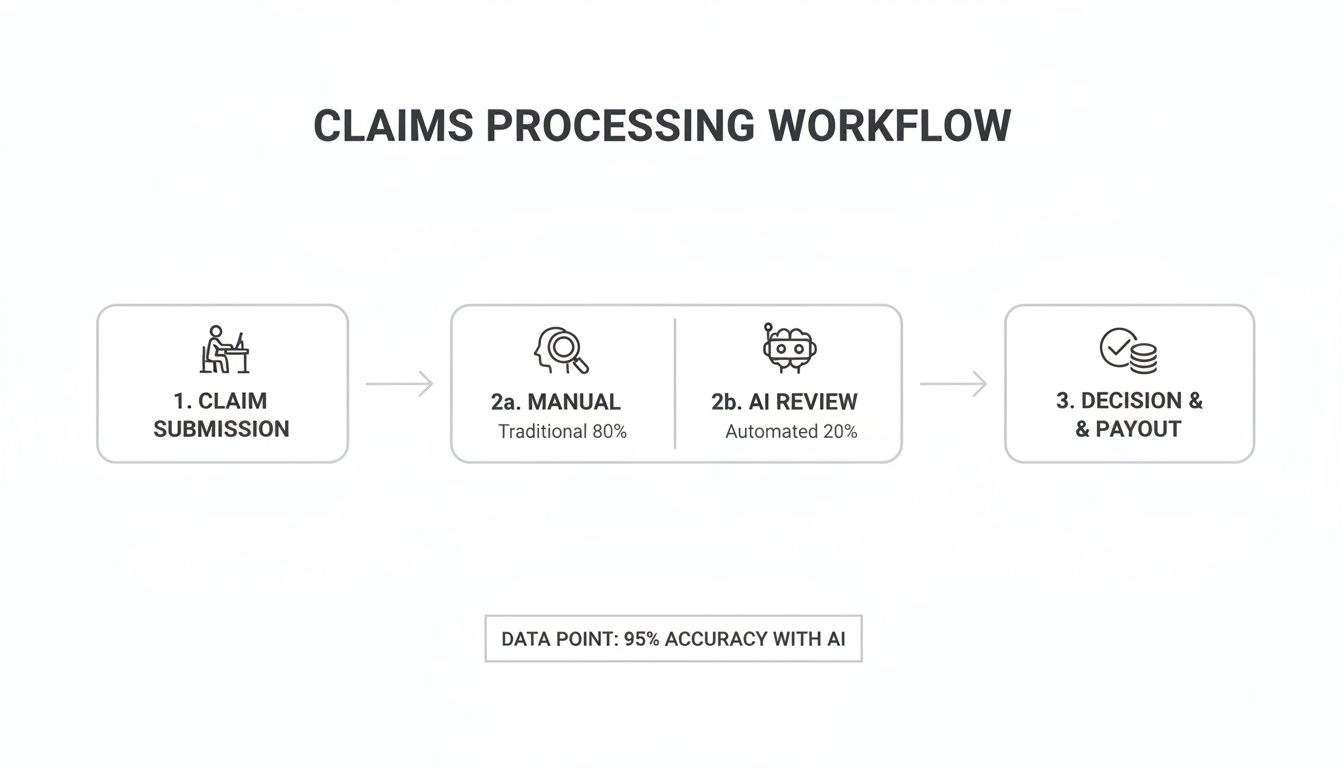
This new flow cuts out the manual handoffs and double-checking, hitting high accuracy levels while making that initial review stage dramatically faster.
Step 2: Automated Evidence Tagging and Categorization
Once all the documents are in one place, the real intelligence kicks in. Instead of a human adjuster slogging through hundreds of pages, an AI model trained on millions of legal and insurance files takes over. This is where that "expert paralegal" analogy really hits home.
In just a few minutes, the AI accomplishes several critical tasks:
Categorization: It instantly identifies and sorts documents by type—a police report here, a medical bill there, a property estimate, a witness statement.
Evidence Tagging: It actually reads the content of each document and applies smart tags, like "liability disputed," "property damage," or "bodily injury."
Data Extraction: It pulls out crucial information—dates, names, policy numbers, dollar amounts—and organizes it into structured data that’s easy to analyze.
This automated tagging turns a mountain of unstructured data into a neatly organized and fully searchable claims file. It’s a process that saves adjusters dozens of hours on every single case.
This isn't just about saving time. It's about creating a consistent, standardized claims file every single time, which is crucial for compliance, audits, and accurate decision-making at scale.
Step 3: First-Pass Risk Scoring and Gap Detection
With all the evidence tagged and organized, the AI platform can give you an immediate "first look" assessment. It analyzes the entire file to generate a claim confidence score, giving you an early read on the claim's complexity and potential risk.
This instant triage helps teams focus their energy where it matters most. A simple, low-risk claim can be sent down a fast track for quick processing. Meanwhile, a complex, high-risk case gets immediately flagged for a senior adjuster to review. For a closer look at how this works, you can learn more about AI for smarter claims triage and decision support.
At the same time, the AI is performing gap detection. It cross-references the evidence on hand against a checklist of everything required for that specific type of claim. If a medical authorization form or a signed affidavit is missing, the system flags it instantly. This simple step prevents the frustrating delays that used to plague the manual process, ensuring the file is complete before it ever lands on an adjuster's desk for a final decision.
The Business Case for AI in Claims Processing
Knowing how AI can rewire a claims workflow is one thing. Seeing how it directly impacts the bottom line is something else entirely. Bringing AI into your claims operation isn't just a nod to modernization; it's a strategic move that delivers real, measurable returns through radical efficiency, lower costs, and much smarter risk management. This is where the theory behind AI becomes cash in the bank.
The value proposition starts by giving your team back its most precious resource: time. We all know that manual claims processing is a notorious time sink, forcing skilled adjusters to burn through their days on low-value administrative grunt work. When you automate tasks like document intake, sorting, and initial review, you hand those hours back to your experts. They can then pivot to high-impact activities—negotiation, complex case strategy, and client communication—that directly improve the quality and speed of every resolution.
Slashing Costs and Reducing Claim Leakage
One of the most powerful arguments for AI is its direct assault on operational costs and claim leakage—the quiet drain of money from inefficient processes or simple human error. Early adopters are already seeing cost reductions between 20-40%, and those savings come from a few key places.
First, AI dramatically shrinks the claim lifecycle. By automatically flagging missing documents or providing instant risk assessments, it cuts out the endless back-and-forth that bloats administrative overhead. Faster resolutions mean fewer billable hours and lower operational costs on every single file.
Claim leakage often happens in small, hard-to-track increments, but it adds up to a significant financial drain. AI acts as a safeguard, ensuring process consistency and accuracy that plugs these leaks, directly protecting your profitability.
Second, the accuracy boost from automation prevents expensive mistakes. A tiny data entry error or an overlooked detail in a medical report can easily snowball into overpayments or unnecessary litigation down the road. AI ensures that claims are handled based on a complete and correctly interpreted set of facts, minimizing these preventable losses.
Uncovering Fraud and Mitigating Risk
Insurance fraud is a massive, multi-billion-dollar problem. Traditional detection methods are often a step behind sophisticated schemes, and it's no fault of the adjusters. No human, no matter how experienced, can possibly connect the dots across thousands of claims to spot subtle, coordinated fraud rings. But AI is built for exactly that.
By crunching immense datasets, AI models can surface anomalies and hidden connections that are invisible to the naked eye. It could be a specific medical provider appearing across an unusual number of unrelated claims or suspiciously similar narratives in accident reports filed months apart. This capability shifts fraud detection from a reactive, after-the-fact exercise to a proactive, real-time defense. With the U.S. alone losing an estimated $308.6 billion to insurance fraud each year, an AI-powered defense is no longer a luxury—it's essential.
The results speak for themselves:
Faster Document Collection: Organizations report gathering claim documents up to 77% faster.
Quicker Resolutions: Claims are often resolved up to four times faster, which frees up reserves and improves cash flow.
Enhanced Adjuster Productivity: Teams can manage higher claim volumes without having to increase headcount, allowing for efficient scaling.
Ultimately, building the business case for AI comes down to connecting the technology to these tangible outcomes. To dig deeper, you can explore the top benefits of automated insurance claims, which cover everything from efficiency and accuracy to major cost savings. The investment isn't just in software; it's in building a more resilient, profitable, and competitive claims operation.
A Practical Roadmap for Implementing AI Claims Technology
Bringing a new technology platform into your operations can feel like a massive undertaking. The key is to break it down. A successful rollout of AI insurance claims processing isn't about flipping a switch overnight; it's about smart planning, step-by-step execution, and a real commitment to helping your team make the shift. And it all starts with an honest look at where you stand today.

The first real step is to map out your current claims workflows. I mean, every single touchpoint, from FNOL to final payment. This process will shine a light on the biggest pain points, bottlenecks, and the manual grunt work that’s slowing everyone down. Are your adjusters burning hours just trying to find the right document? Are you constantly chasing down missing information?
Getting specific about these problems gives you clear targets. Your goal isn't just to "implement AI." It's to solve real-world business challenges, like shrinking cycle times, slashing administrative overhead, or just making your claim files more consistent and reliable.
Phase 1: Initial Planning and Vendor Selection
Once you know exactly what problems you're trying to solve, you can start looking for the right partner. Not all AI platforms are created equal, so you need to find one whose tech actually lines up with your specific P&C needs. Start by building a scorecard of your must-haves.
A few non-negotiables to put on your list:
Domain-Specific Training: The model absolutely has to be trained on relevant P&C and legal data, not generic web content. This is a deal-breaker.
Seamless Integration: The platform has to play nice with your existing claims management system (CMS). The last thing you want is another data silo.
User-Friendly Interface: If the tool is clunky or confusing, your adjusters won't use it. It needs to make their lives easier, not harder.
And let’s be clear: security has to be at the very top of that list. An enterprise-grade platform isn't optional. Look for vendors with certifications like SOC 2 and HIPAA readiness. That’s your proof that they take protecting sensitive claims data seriously with rigorous, audited security controls.
Phase 2: Data Integration and Pilot Program
After you’ve picked a vendor, the focus shifts to data. This is where you connect the AI platform to your systems and, most importantly, launch a pilot program. A pilot is your chance to test-drive the technology in a controlled setting before going all-in.
Choose a small, representative team or a specific group of claims for the test run. This lets you iron out any integration wrinkles, get early feedback from the folks who will actually use the tool, and measure the impact on a manageable scale. The lessons you learn here will make the full, company-wide launch infinitely smoother. For teams drowning in paperwork, you might want to dig deeper with our practical guide to AI document review.
Phase 3: Change Management and Full Rollout
Here’s a hard truth: technology is only half the battle. The other half is your people. The number one reason new tech initiatives fail is a lack of user adoption. That's why effective change management is so critical to getting this right.
You have to frame the AI correctly. It’s not a replacement for your adjusters; it’s a powerful assistant built to handle their most tedious, soul-crushing tasks. The message should be about freeing them up to focus on the high-value work that requires a human touch—like complex analysis, negotiation, and strategic decision-making.
Provide great training, identify internal champions who can help their colleagues, and be completely transparent about the goals. A successful rollout depends on turning your team from skeptics into the platform’s biggest advocates.
Real-World AI Use Cases and Outcomes
The true test of any technology isn't in its features list—it's how it performs under pressure. For P&C carriers, TPAs, and law firms, the value of AI insurance claims processing becomes crystal clear when you see it solve specific, high-stakes problems and deliver results you can measure.
Let's move past the theory and into the trenches. Here are tangible before-and-after scenarios where AI completely reshapes outcomes.

These stories aren't just about efficiency. They show how AI platforms can turn chaotic, high-volume situations into controlled, strategic operations, painting a vivid picture of the ROI.
Managing a Surge in Catastrophe Claims
Imagine a major hailstorm hammers a dense suburb, burying a regional P&C carrier in thousands of property damage claims in just 48 hours. This is a classic catastrophe (CAT) event—and an operational nightmare.
Before AI: The claims team is instantly underwater. Phones are ringing off the hook while inboxes flood with photos, contractor estimates, and frantic messages. Adjusters are stuck working overtime, manually downloading attachments, creating new files, and just trying to keep track of who sent what. The whole process is slow, inconsistent, and riddled with the risk of error as everyone rushes to keep up. Policyholders are frustrated, and the backlog grows by the hour.
After AI: This time, the carrier routes every incoming claim through an AI intake system. The platform acts as an instant digital command center, ingesting every email, photo, and PDF and organizing the data on a single dashboard.
Instead of a frantic manual scramble, the AI gets to work instantly:
It Identifies Document Types: The system knows the difference between a contractor's bid, a photo of roof damage, and a policy endorsement.
It Extracts Key Data: Policy numbers, incident dates, and damage descriptions are pulled out and structured automatically.
It Flags High-Priority Cases: Claims showing signs of severe structural damage are automatically flagged and routed to a senior adjuster for immediate review.
The result? A calm, organized response. The team can see the full scope of the event in real-time, prioritize the worst-hit properties, and proactively communicate with policyholders. The AI handles the administrative storm, freeing up adjusters to focus on evaluation and settlement.
This shift transforms a reactive crisis into a structured, scalable response. The carrier reduces document collection time by 77% and starts resolving claims days, not weeks, after the storm.
High-Volume Workers' Compensation for a TPA
Now picture a third-party administrator (TPA) that manages thousands of workers' compensation claims for several large clients. Each case is a mountain of paperwork—medical records, incident reports, wage statements, you name it. Their biggest headache is processing this sheer volume efficiently while maintaining pinpoint accuracy and compliance.
Before AI: The TPA’s workflow is a series of slow, manual handoffs. An admin team spends all day sorting and labeling incoming medical bills and reports. Adjusters then have to read through every single document, hunting for key information like treatment dates or disability status. It’s not just time-consuming; it's a minefield for costly errors. Missing one critical detail buried in a 200-page medical narrative could change the entire direction of a claim.
After AI: The TPA implements an AI claims intelligence platform that’s been trained on medical and legal documents. Now, when that 200-page medical file arrives, the system does the heavy lifting in minutes.
Automated Medical Tagging: The AI instantly identifies and tags crucial concepts like "Maximum Medical Improvement (MMI)" or "Permanent Partial Disability (PPD)" and even specific medical procedures.
Gap Detection: The system cross-references the file against state requirements and flags if a mandatory medical authorization form is missing.
Instant Summarization: It generates a clean, concise summary of the medical timeline. The adjuster gets a complete overview without having to read every single page.
This automation lets the TPA handle a much higher volume of claims without hiring more people. Adjusters are no longer document detectives; they’re strategists who receive organized, pre-analyzed files ready for their expertise. This leads to a 4x improvement in claim resolution speed, slashing administrative costs and dramatically improving service levels for their clients.
These scenarios prove that AI isn't just about making small tweaks. It’s about creating fundamentally better, smarter ways to manage risk and serve customers.
How to Choose the Right AI Partner for Your Needs
Picking an AI platform for claims isn't like buying off-the-shelf software. It’s a strategic partnership. The market for AI insurance claims processing is incredibly crowded, and frankly, not all solutions are built to handle the messy reality of P&C claims. A flashy demo doesn't mean much if it can't deliver in the real world, so you have to look past the marketing hype and focus on what actually drives value.
The right partner gives your team a tool that makes them better at their jobs, plugs into your existing systems without a fuss, and produces consistent, audit-ready work. This guide is a no-nonsense checklist to help you ask the right questions and pick a vendor that genuinely fits your operation.
Focus on Domain-Specific Intelligence
This is the single most important factor. An AI model trained on generic internet data is useless for claims. It will completely miss the nuance in insurance policies, medical records, and legal documents. It’s like asking a general practitioner to perform brain surgery—they understand the basics of medicine, but they lack the critical, specialized expertise.
For an AI to actually work, it must be trained on domain-specific P&C and legal data. This is non-negotiable. This training ensures the platform can accurately:
Tell the difference between a police report and a medical bill without getting confused.
Spot key insurance concepts like subrogation potential or liability.
Understand industry jargon and the context behind it.
Without this specialized intelligence, the AI will spit out unreliable results, creating more work for your team, not less.
Prioritize Security and Seamless Integration
Your claims data is incredibly sensitive, so rock-solid security is a dealbreaker. Any partner you consider has to prove they take this seriously with enterprise-grade security.
Look for vendors with verifiable certifications like SOC 2 Type II. This isn't just a piece of paper; it's proof they’ve passed rigorous, independent audits of their security controls. And if you handle any claims with medical information, HIPAA readiness is an absolute must.
The platform also needs to play well with your current Claims Management System (CMS). An AI tool that operates in its own little bubble is a step backward. The whole point is to create a seamless flow of information that makes your current workflow smarter, not to add a clunky tool that forces your team to copy and paste data all day. True integration means the AI feels like a natural extension of your operational backbone, feeding structured data right where you need it.
Fraud detection is another area where a great AI partner earns its keep. AI can spot complex patterns that even experienced adjusters might miss, directly protecting your bottom line. It's not just talk—McKinsey data shows early AI adopters have seen 20-40% cost reductions in claims, a huge chunk of which comes from better fraud prevention. A recent survey backs this up, with 79% of claims professionals now focused on documentation automation to hit that kind of ROI. You can dig deeper into AI's impact on the insurance industry to see where things are headed.
Common Questions About AI in Claims Processing
Even with a clear roadmap, it’s natural to have questions when you’re looking at bringing in new technology. When it comes to AI in insurance claims, most of the conversations I have with leaders eventually turn to the impact on people, data security, and what the real-world return on investment actually looks like.
Let’s tackle these head-on and clear up some of the noise around this technology.
Will AI Replace Our Claims Adjusters?
No. The goal isn't to replace adjusters, but to make them better at their jobs. Think of it this way: AI is fantastic at the high-volume, repetitive work that burns out your best people—sorting documents, pulling out key data, and doing that first-pass review.
Freeing your adjusters from that low-value work means they can shift their energy to the things that actually require a human brain:
Complex Case Strategy: Untangling the knotty, nuanced situations that no algorithm can solve.
Negotiation: Having the tough, empathetic conversations needed to reach a fair settlement.
Customer Interaction: Providing the human support that builds trust and keeps policyholders loyal.
I like to think of AI as a powerful co-pilot. It handles the monotonous systems checks, allowing the pilot—your adjuster—to focus on navigating the complex journey ahead. It’s all about empowering your team, not sidelining it.
How Secure Is Our Claims Data with an AI Platform?
In this industry, security is completely non-negotiable. The top AI platforms are built from the ground up with enterprise-grade security as their foundation. When you’re vetting vendors, this is where you need to get serious and ask for proof.
Look for vendors with SOC 2 certification. This isn't just a logo on a website; it means they've undergone a rigorous, independent audit of their security controls and processes. For any enterprise-level partnership, it's a critical benchmark.
And if you're handling claims with any health information, HIPAA readiness is an absolute must. These certifications are your assurance that sensitive claims data is locked down with audited, proven safeguards against breaches and unauthorized access.
What Is the Typical ROI for AI Claims Processing?
The return on investment shows up in a few different, powerful ways. We see organizations resolving claims up to four times faster and cutting the time spent just collecting documents by a staggering 77%. That kind of speed has a direct impact on operational costs and helps plug claim leakage.
Some early adopters have reported cost reductions of 20-40% in their claims operations. The ROI isn't just a single number; it's a combination of greater efficiency, smarter fraud detection, and giving your adjusters the leverage to handle more volume without needing to add headcount.
Wamy is an AI claims intelligence platform that turns raw claim data into confident, audit-ready decisions. Centralize your intake, automate evidence review, and resolve claims up to 4x faster. Discover the difference.